Dr. Med. Victor N. Solopov
For over one hundred
years, asthma and allergy have been inextricably linked. Whenever asthma
is discussed, allergy is invariably mentioned, but until recently the
key question remained unanswered: Does allergy cause asthma, or do they
coexist, developing independently of each other?
The international
committee of experts at GINA 2002, tried to establish a causal
relationship between allergy and asthma, but were forced to admit
defeat. Here are some quotes from the GINA 2002 report:
1. “However,
when expressed in the lower airways, atopy is one of the strongest risk
factors for asthma.” (p. 4). At the same time one can find: “Atopy
occurs in 30 to 50 percent of the population in developed countries and
frequently occurs in the absence of disease” (p. 4).
2. “Asthma… is
frequently found in association with atopy, which is defined as the
production of abnormal amounts of immunoglobulin E (IgE) directed to
episodes expressed on common environmental allergens…” (p. 4). At the
same time”…most studies report an inconsistent association between the
increase of atopy and the increase of asthma” (p. 30).
3. “In many
cases, especially in children and young adults, asthma is associated
with atopy manifesting through immunoglobulin E (IgE) – dependent
mechanisms. At a population level, the contribution of atopy to the
asthma phenotype has been estimated to be 40 percent in both children
and adults.” (p. 50). But “… a third of all cases of asthma could be
categorized as non allergic” (p. 51).
The experts concluded that: “A
major unresolved question is whether exposure to allergens and
occupational sensitizers is indeed the primary cause of the development
of new asthma, or if this exposure merely triggers asthma attacks or
leads to the persistence of symptoms in subjects who already have
asthma” (p. 32). Two conclusions can be formed from the facts presented
in this report:
1. Atopy (allergy) is often combined with bronchial asthma, but in 30-50% of all cases, it does not cause the disease.
2. Despite similar immunological mechanisms in atopy and asthma, atopy cannot be the cause of asthma.
What
are these mechanisms? They are connected by two different
subpopulations of lymphocytes helpers: Th1- and Th2 types. The first
type are responsible for the normal immune response which protects the
human organism from infection. A prevalence of activity of the second
type (Th2- helper subtype) leads to IgE synthesis of antibodies to
different “allergens” – the precise allergen depends on which immune
pathway is affected. When this happens, the immune system starts to
perceive animal hair/fur, pollen, various foodstuffs, medicines, etc. as
“allergens”.
Th2-helpers active in bronchial asthma pathogenesis
produce a number of cytokines such as IL-4, IL-5, IL-9, IL-13 and IL-16.
Th2-cytokines are responsible for classic hypersensitivity delayed-type
reaction (also known as cell-mediated hypersensitivity); and cytokine
IL-5 (produced by Th2-lymphocytes) causes eosinophilous inflammation,
irrespective of the presence of asthma or atopy.
From these facts, it
can be proposed that the factor that gives rise to the inflammatory
process and changes in the immune response from Th1 – to Th2 – helper
path, may be the true cause of asthma. If such a factor exists, the
inflammation caused by it, on the one hand leads to asthma, and on the
other, to atopy (which can aggravate asthma or exist without clinical
symptoms) as a marker of immunity system changes.
What could this
factor be? Clearly, it must be closely connected with the immune system.
As the immune system evolved primarily as a protection against
infection, it is logical to assume that the factor is infectious. As
many physicians know, until recently bronchial asthma was classified as
infectious. In addition, the data shows that the most severe asthma
cases are accompanied by neutrophilous – infectious – inflammation.
Taken together this evidence leads one to ask: 1) Which infection could
it be? and 2) How is it connected with asthma and atopy?
Identification
of the micro-organism should be possible from bacteriological analyses
of sputum and intestinal content of patients. Analyses have shown the
following results:
· Fungal microorganisms are revealed in 69.8 % of all the analyses.
· Candida spp. were found in asthmatics’ sputum in 63.3% of patients.
· Other fungi – Aspergillus and Penicillium – were found in 2.3% and 4.1% of samples, respectively.
·
All these fungal micro-organisms were associated with bacteria:
Streptococci and staphylococci were found in 55.9% and 52.4%
respectively.
· Other bacterial micro-organisms – Klebsiella pneum. and E. Coli – were found in 12.8% and 2.4% respectively.
·
Occasionally other bacteria were found. In particular Pseudomonas spp,
e.g. Pseudomonas aeruginosa were found in 0.087% of all patients’
sputum.
· Fungal micro-organisms were the most prevalent in sputum
bacteriological analyses, and were found in the majority of the patients
under investigation. In almost all cases, Candida was accompanied by
various types of bacteria. Only in one case, was Candida albicans found
without any co-existing bacteria.
· At the same time, Candida was found in 99.6% of the intestinal content of the asthmatics under study.
It
should be noted that Candida. spp are often found in healthy people. In
particular Candida albicans is a saprophyte commonly found on human
skin, the oral cavity and mucosa. Its prevalence in the general
population is as follows: on the skin (19-70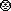 ; in the oral cavity of
adults (20-30
; in the oral cavity of
adults (20-30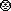 ; in newborns’ oral cavities (90
; in newborns’ oral cavities (90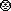 ; in the intestinal
tract of adults (36
; in the intestinal
tract of adults (36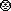 , and in the intestinal tract of children (50
, and in the intestinal tract of children (50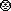 .
Thus, according to the literature and our own data, most people with
bronchial asthma have Candida spp. in their sputum and intestines.
.
Thus, according to the literature and our own data, most people with
bronchial asthma have Candida spp. in their sputum and intestines.
When
analyzing this data, we found a direct correlation between the increase
in Candida spp. and the rise in asthma over the last 50 years. Fifty
years ago, the number of Candida carriers in Russia was 5-15% of the
population, and the asthma frequency was 0.1-0.5%.
In the 1960-1980s
these indices increased so that the percentage of Candida carriers
became 20-53% and asthma frequency reached 1-3% of the whole population.
During
1990-2001 the percentage of Candida carriers and asthmatics reached on
average 60-70% and 4-15% of the whole population, respectively. Thus,
both of these indices have grown concurrently over these years, not less
than 5-10 times.
When Candida micro-organisms settle on the human
mucosa in unhealthy situations (caused by massive antibiotic therapy,
local immune system weakness etc.) they start active colonization, and
produce toxins that cause epithelium damage. Some Candida toxins can
liberate histamine from mast cells leading to initial mucosal
inflammation, and further immune system reactions.
Candida
reproduction and excretion of its toxins can cause an initial
inflammatory process, which can be neutrophilous In addition, the
presence of Candida increases the pathological action of other microbes,
which exacerbates the inflammatory process in the respiratory tract
mucosa. The further mutation of Th1-helper to Th2-helper leads directly
to eosinophilous inflammation and the development of asthma. Data from
the scientific literature confirms that Candida fungal infection is
capable of “switching” the immune system from normal (Th1-helper) to the
pathological Th2-helper response.
Asthma inflammation may be an
attempt by human immune cellular mechanisms to “crash” release from
massive fungal Candida colonization, in order to avoid severe damage
from phagocytosis. As a result its immunity is compelled to pass on the
less damaging – antibody productive way – with participation of
Th2-helper lymphocytes, which leads to atopy. Generated atopy causes
acute allergic (antibody-mediators) reactions to different allergens in
the organism, shown by paroxysmal bronchial spasm against a background
of an inflammatory process persisting in the bronchial tree.
Inflammatory reactions of the cellular-mediated type with participation
of T-lymphocites-killers simultaneously proceed in the bronchial tree.
As is known, they develop in those cases where the immune system meets
antigens on the surface of alien cells.
In summary, it is possible
that the true cause of bronchial asthma development could be Candida
yeast-fungi. These microorganisms are considered to be saprophytes
living in the mouth and human intestinal tract. Their uncontrollable
reproduction and colonization on the intestinal tract mucosa induces a
change in immune response from Th1- to Th2-helper, and that leads to
atopy. Its penetration to the respiratory tract with associated bacteria
may induce initial neutrophilous inflammation. The consequential change
from Th1- to Th2-helper immune response transforms the inflammatory
process to an eosinophilous type, that leads to bronchial asthma
Consequently, atopy can exist without asthma, and asthma without atopy.
When they do combine, atopy can exacerbate the inflammatory process in
the bronchial tree, helping to turn it into a chronic condition
The
asthma and allergy growth rates may be induced by frequent antibiotic
treatment of patients. Looking again at the frequency data of Candida
and asthma in different years, it is noticeable that their growth
coincides with the beginning of medicinal usage of wide-spectrum
antibiotics at the end of the 1950s and beginning of 1960s. This
observation supports the famous monograph “Candida mycosis as a
complication of antibacterial treatment” written by A. Arievich and Z.
Stepanishcheva.
The present day level of incidence of Candida in
healthy people (70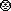 cannot be considered to be normal. Local and
systemic candidiasis have spread to such a degree, that wide-spectrum
antifungal preparations are advertised in the mass media. When
considering all of these facts together, it becomes clear why the
international experts committee GINA 2002 came to following conclusion:
“Despite efforts on improvement of rendering assistance in patients with
BA undertaken within last decade, the majority of patients has not
received advantage of achievements in this field”. It is no coincidence
that all three factors: the wide beginning of antibiotics treatment,
growth of Candida carrier level and a bronchial asthma rate growing, are
observed over the same period.
cannot be considered to be normal. Local and
systemic candidiasis have spread to such a degree, that wide-spectrum
antifungal preparations are advertised in the mass media. When
considering all of these facts together, it becomes clear why the
international experts committee GINA 2002 came to following conclusion:
“Despite efforts on improvement of rendering assistance in patients with
BA undertaken within last decade, the majority of patients has not
received advantage of achievements in this field”. It is no coincidence
that all three factors: the wide beginning of antibiotics treatment,
growth of Candida carrier level and a bronchial asthma rate growing, are
observed over the same period.
The infectious nature of asthma
explains another fact. It is well known that fungal infections can be
transferred within households. It has also been observed that asthma is
passed among contacts who are not blood relatives, for example between
husband and wife. This is inexplicable in terms of heredity, but
explained by a fungal infection. It also explains why twins suffer more
than brothers and sisters – the probability of simultaneous infection
with Candida from mother to twins is higher. This explains the
unsuccessful attempts to connect asthma with heredity, and it even
explains why one can observe cases of asthmatic twins where one is sick
and the other is absolutely healthy.
One can ask a general question:
should every person be infected with Candida microorganisms? Clinical
and epidemiological research done in 1950 show that yeast fungi Candida
were found in the mouth and pharynx of healthy people, in less than 5%
of the population. Undoubtedly the uncontrolled growth of these
pathogenic microorganisms has had a detrimental effect on public health.
It appears that microorganisms in general are implicated as a cause of
many non-specific inflammatory diseases, not just asthma, and play a
more important role than is currently considered. This particularly
applies to those cases where bacteria and fungi act on human organs and
systems not by “frontal” attack as, for example, in purulent diseases,
but in a more refined way – by switching the immune system response from
normal to pathological.
We need to revise our view of how people and
microbes live together symbiotically, with both “partners” following
the rules of the game. That revision could lead to a change in our
general model of causality in medicine.
Dr. Victor. N. Solopov
Translated from: The “Medical Newspaper”, (Moscow), N 54, 21. 07. 2006